Could AI Help Improve Outcomes and Reduce Medications?
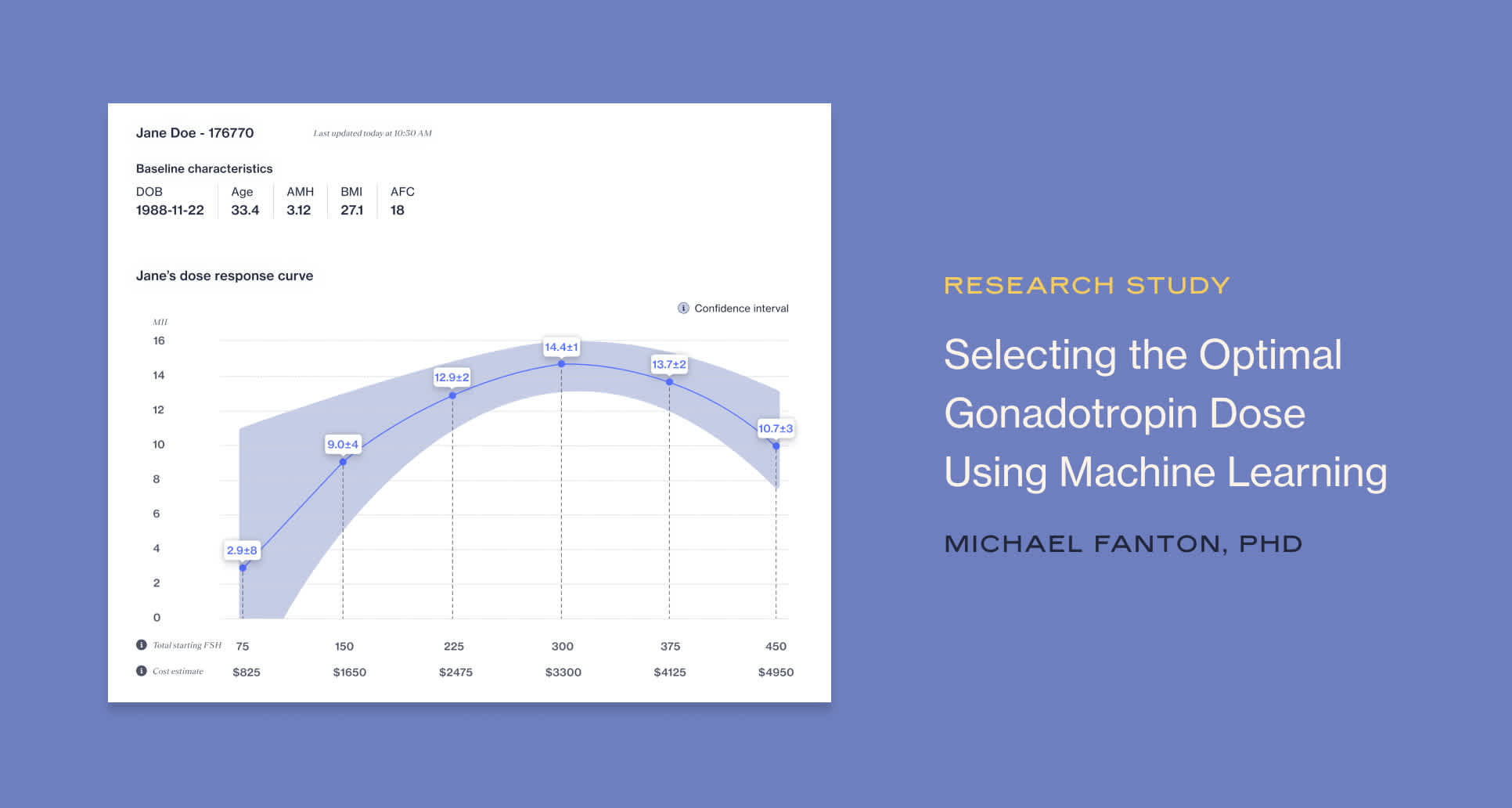
Alife Data Scientist Michael Fanton, PhD, presented his research “Selection of optimal gonadotropin dose using machine learning may be associated with improved outcomes and reduced utilization of FSH” to a live audience at the 2022 American Society of Reproductive Medicine conference this October. Michael’s research contributed to the development of Stim Assist™, part of the suite of the Alife Assist™ platform, that provides physicians and fertility clinic operators with AI and data-driven insights to optimize each step of the IVF process.
We were excited to chat with Michael about the role gonadotropins – hormones that are used to treat infertility – play in ovarian stimulation during IVF. We also talked with him about how artificial intelligence (AI) can help doctors personalize medication doses during a patient’s IVF cycle, and the impact that the number of eggs retrieved per cycle has on outcomes.
For more information on ovarian stimulation during IVF, how machine learning can help optimize egg retrieval, and IVF medication costs, be sure to check out our blog!
Interview with Michael Fanton, PhD, Alife Data Scientist:
What is gonadotropin? What does it do to the body?
Ovaries contain small fluid-filled sacs called follicles. During a natural menstrual cycle, one dominant follicle in the ovary will develop and release a single mature egg. However, during an IVF cycle, a patient will want to retrieve as many eggs as possible to maximize their chances of having a live birth. Gonadotropins are injectable hormones given to patients to promote the development of multiple follicles in the ovaries so that multiple eggs can be retrieved. The two types of gonadotropins that are given during IVF are follicle stimulating hormone (FSH) and luteinizing hormone (LH).
At what point during an IVF cycle is a gonadotropin dose given?
Gonadotropins are given during ovarian stimulation, which is the first stage of IVF. During this process, a patient will take daily injectable gonadotropins as the follicles mature, generally for around 8-14 days.
Why is it important to reduce use of FSH?
In the United States, patients are commonly prescribed between 100 and 600 international units (IUs) of daily FSH during ovarian stimulation. Too little FSH may result in not enough stimulation and thus few eggs retrieved, while too much FSH can result in ovarian hyperstimulation syndrome (OHSS), a condition caused by an excessive response of the ovaries. Recent data has shown that for many patients, giving more FSH does not actually make the ovaries respond better, and therefore will not improve outcomes. If there is no benefit to higher doses, then using lower doses of FSH could help reduce the number of injections and overall cost of medications for patients, which in some cases could add up to thousands of dollars.
How can AI help to select the optimal dose of FSH? How can doctors use this information to help reduce FSH and improve IVF outcomes?
We can use AI to personalize the dose of FSH to each patient based on their baseline fertility characteristics. To do this, the AI analyzes data from tens of thousands of prior cycles from multiple different IVF clinics and creates a model of how an individual is expected to respond to different doses of FSH. With this model, the doctor can see which patients are likely to respond to higher doses of FSH, and then select what they feel is the optimal dose for a specific patient.
Does maximizing the number of eggs per retrieval cycle really help outcomes, or can it result in lower quality eggs?
We have analyzed over 90% of all cycles that occurred in the US between 2014-2019 and found that retrieving more eggs, on average, is associated with a higher cumulative live birth rate. The cumulative live birth rate is the most relevant metric for a patient because it takes into account the chances of having a baby from all of the eggs retrieved from a cycle. The reason for this is pretty intuitive - more eggs means that there are more opportunities to transfer embryos, and thus a higher chance of a successful pregnancy. There have been older studies which have suggested that retrieving too many eggs may be detrimental to egg quality. Our analysis of more recent data shows that this is not the case - egg quality does not appear to decline at higher egg yields.
For physicians and clinic operators, please reach out for a demo of Stim Assist – a set of AI-powered tools that enable reproductive endocrinologists to combine their clinical expertise with insights gathered from tens of thousands of past patient cycles to optimize starting dose of FSH and trigger day during a stimulation cycle. We’re always glad to hear from you!
Recent Articles
Share this
Recent Articles

Learn everything you need to know about IVF
Join the newsletter for IVF education, updates on new research, and early access to Alife products.



Sign up for our newsletter for the latest advancements in fertility care.
©2026 by Alife Health
Terms
Privacy
App Privacy
Security
Cookie Declaration
[website version: 740-00200-REC-01 Rev 2]
