Egg Freezing Success Rates

Medically reviewed by Linda Streety, RN, BSN
If you would like to be proactive about your fertility, you may consider a form of fertility preservation known as “egg freezing.” When you freeze your eggs, you use hormone medications to stimulate your ovaries to produce multiple eggs (usually about 10-20), have them retrieved in a simple, outpatient procedure, and then freeze them at a storage facility for later use.
Below we’ll talk about the factors that affect your chance of success, egg freezing success rates by age, how many eggs you should freeze, and what to consider when deciding whether to freeze eggs or embryos.
Factors that may affect your chance of success with frozen eggs
How your eggs were frozen
Freezing techniques have improved a great deal in recent years. Previous cryopreservation freezing techniques tried to avoid ice crystal formation in eggs by slow freezing them, a technique that resulted in many lost eggs from damaged cell walls. Currently, most eggs are frozen using vitrification, a flash freezing technique that results in a high percentage of eggs surviving thawing (92-97%) and equivalent fertilization rates as with fresh eggs (1). (Note that this thaw survival rate is from research conducted in 2011, and since freezing techniques have improved, this rate may have improved.)
Your age at the time of egg retrieval
A major reason why people choose to freeze their eggs is that fertility declines with age. Egg freezing suspends eggs at the age at which they were retrieved, improving your chance of success with IVF should you choose to use those eggs in the future.
The number of mature eggs retrieved
While researchers used to believe there was a maximum number of eggs you could retrieve during a cycle before harming outcomes, new research shows otherwise. Research conducted by Alife data scientists found that the more eggs your clinician is able to retrieve after an ovarian stimulation cycle, the better your chance of success with IVF.
Factors that should not affect your chance of success with frozen eggs
Your age at the time of embryo transfer
While maternal age does correlate to a decline in egg quality, it doesn’t necessarily affect the uterus’s ability to carry a child. One study of donor eggs compared implantation and pregnancy rates among patients 39 years of age or less and patients 40-52 years old, and found no significant differences between them (2). That said, some researchers have found that after age 45, implantation and pregnancy rates decrease (3).
How long your eggs have been frozen
A study of frozen then thawed eggs found that the length of time that eggs had been frozen had no impact on a patient’s chance of IVF success with them (4).
How many eggs should I freeze for my age?
Because egg quality declines with age, you may need to freeze more eggs if you are older in order to improve your chance of a successful pregnancy. Below is a chart that shows your probability of having a live birth vs. the number of mature eggs you would have to freeze by age (5).
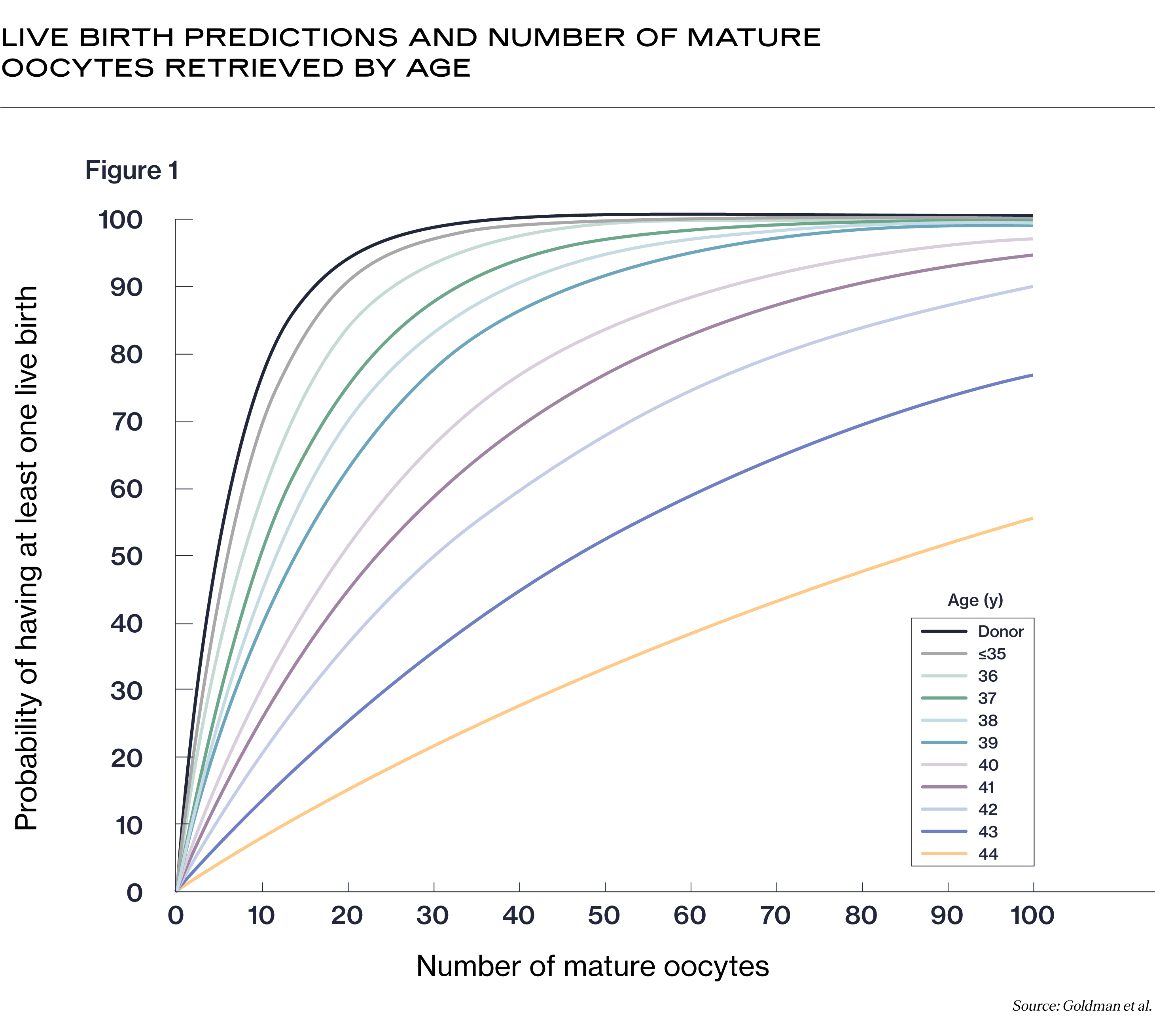
As you can see in the graphic above, the ideal number of eggs (also known as "oocytes") you need to freeze increases as you age. While someone under 35 may only need to freeze 10 eggs for a 70% chance of success with IVF, someone around 40 years old would need closer to 34 eggs for the same chance of success.
Unfortunately, though you need more eggs to improve your chance of success as you age, the average number of eggs you are likely to retrieve decreases with your age.
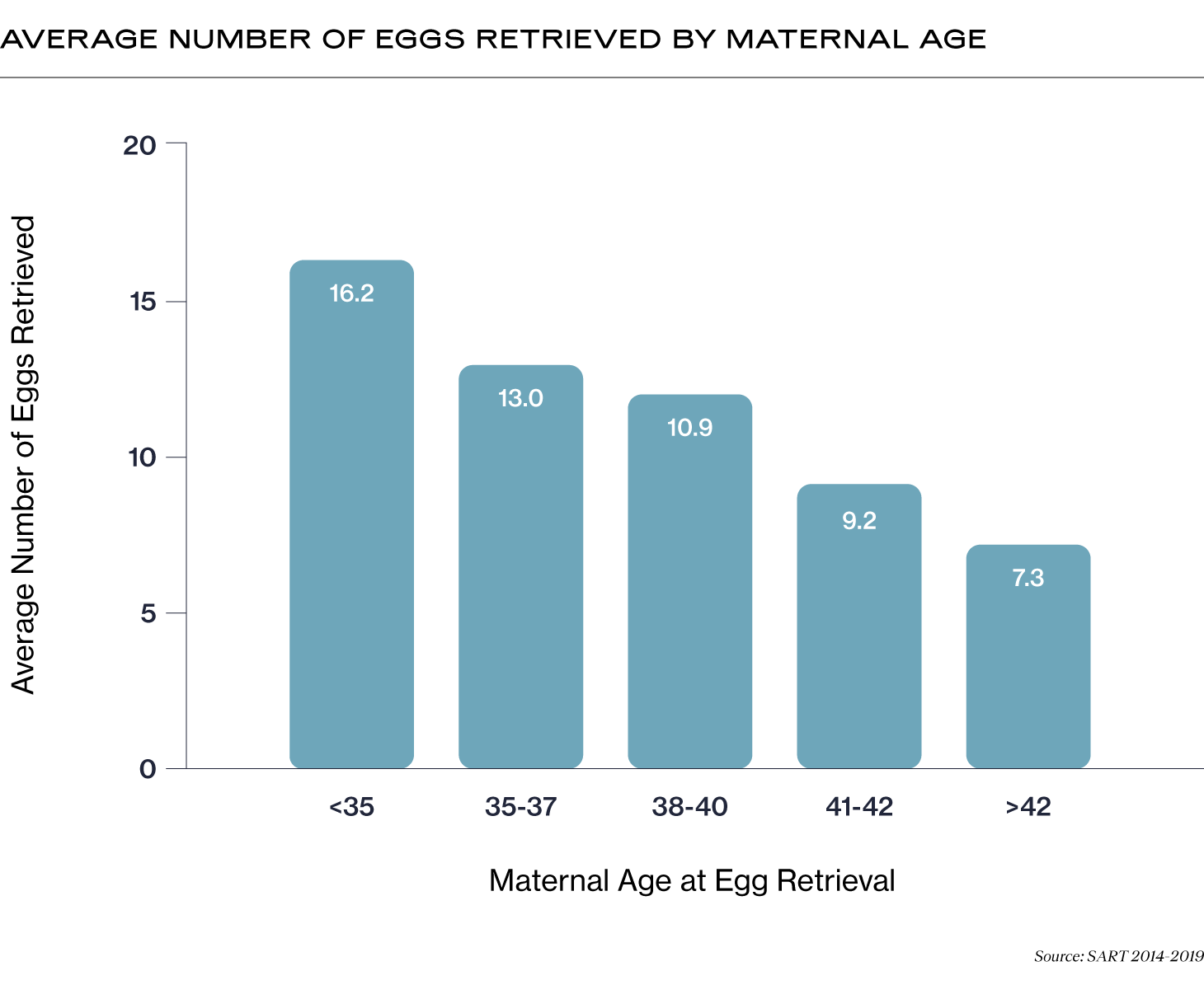
Again, we want to emphasize that each body is different, so the number of eggs you retrieve may differ from this chart. Knowing your particular anti-müllerian hormone levels (AMH) and antral follicle count (AFC) can help you better understand your individual chance of success. Additionally, since some of your retrieved eggs may not yet be mature, the number of eggs you can freeze will likely be lower than the number of eggs your RE retrieved.
What are the egg freezing success rates by age?
Many people who undergo IVF need more than one cycle in order to have a baby. Since egg freezing usually means that you plan to use the eggs in the future, you may not know how successful your outcomes will be for many years. Below is a chart that shows your chance of a live birth with 1 or 2 egg freezing cycles (6).
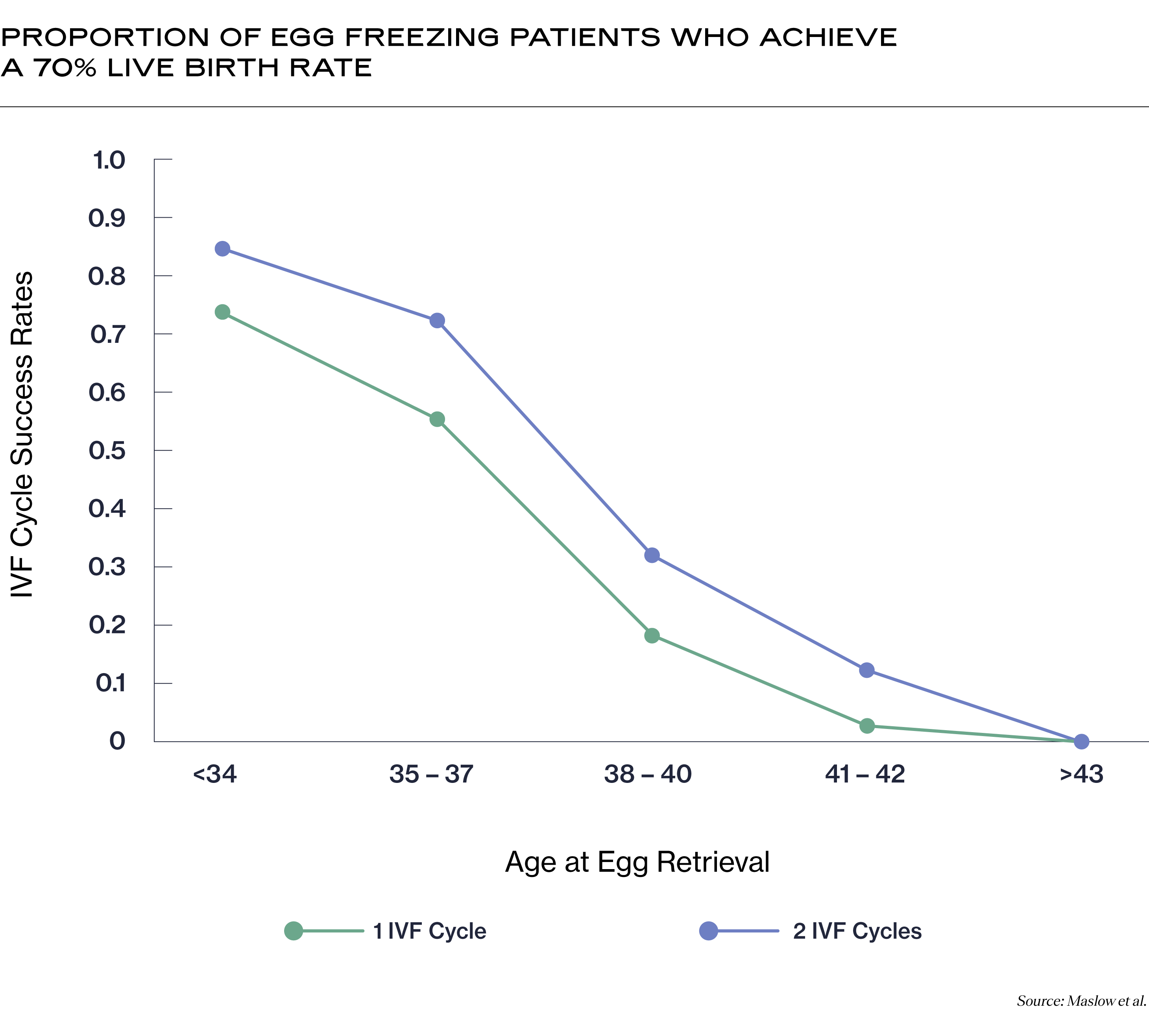
An important takeaway from all this information is that egg freezing is a form of fertility preservation that improves your chance of having a baby through IVF in the future by “freezing” your eggs at a certain age. However, it is not necessarily a guarantee that you will have a baby with those eggs in the future.
You may also end up conceiving naturally or through intrauterine insemination (IUI) and may not need to use your stored eggs.
Should I freeze eggs or embryos?
This is a complex question to answer. Let’s start by thinking about the IVF “funnel.” Because IVF is a process involving many steps – ovarian stimulation, egg retrieval, fertilization, embryo culture, then embryo transfer – some eggs or embryos are usually lost at each step. Freezing eggs adds a point of potential loss to this process, since about 3-8% of eggs may be lost when they are thawed. However, there’s more to consider than just this:
The case for freezing embryos
If you have an opposite sex partner that you plan to have children with, or you plan to use donor sperm regardless of when you choose to do embryo transfer, then creating and freezing embryos is a good choice. This eliminates a potential point of loss (egg freezing and thawing).
An embryologist can also assess embryo quality much more thoroughly than they can assess egg quality. This gives them a sense of each embryo’s ability to implant and grow into a healthy baby. If you choose to, the embryologist can also conduct preimplantation genetic testing (PGT-A) on the embryos to ensure that they are chromosomally normal, a step that can’t be taken yet with eggs. All this extra information could give you a better sense of your chance of success with IVF and help you decide whether you should do another round of ovarian stimulation to optimize your chance of having a baby later on.
The case for freezing eggs
If you don’t currently have an opposite sex partner or you don’t want to use donor sperm, egg freezing allows you greater flexibility in the future to build a family in a way that’s best for you. It also avoids a potential legal battle with a partner if you split up before using the embryos (sperm donors relinquish their rights to parenthood so this would not be an issue with embryos created through sperm donation!) If chromosomal abnormalities are a concern, you can conduct PGT testing later after thawing and fertilizing your eggs.
Only you can decide whether it’s better to freeze eggs or embryos. However, equipped with information about your chance of success with either, you can decide the right path for you.
Recent Articles
References
-
Cobo, A., & Diaz, C. (2011). Clinical application of oocyte vitrification: a systematic review and meta-analysis of randomized controlled trials. Fertility and Sterility, 96(2), 277–285. https://doi.org/10.1016/j.fertnstert.2011.06.030
-
Abdalla, H. I., Wren, M. E., Thomas, A., & Korea, L. (1997). Age of the uterus does not affect pregnancy or implantation rates; a study of egg donation in women of different ages sharing oocytes from the same donor. Human Reproduction, 12(4), 827–829. https://doi.org/10.1093/humrep/12.4.827
-
Soares, S. R., Troncoso, C., Bosch, E., Serra, V., Simón, C., Remohí, J., & Pellicer, A. (2005). Age and Uterine Receptiveness: Predicting the Outcome of Oocyte Donation Cycles. The Journal of Clinical Endocrinology & Metabolism, 90(7), 4399–4404. https://doi.org/10.1210/jc.2004-2252
-
Torra-Massana, M., Miguel-Escalada, I., Vassena, R., & Rodríguez, A. (2023). Long-term storage of vitrified oocytes does not affect pregnancy and live birth rates: analysis of 5362 oocyte donation cycles. Reproductive BioMedicine Online, 103228. https://doi.org/10.1016/j.rbmo.2023.04.019
-
Goldman, R. H., Racowsky, C., Farland, L. V., Munné, S., Ribustello, L., & Fox, J. H. (2017). Predicting the likelihood of live birth for elective oocyte cryopreservation: a counseling tool for physicians and patients. Human Reproduction, 32(4), 853–859. https://doi.org/10.1093/humrep/dex008
-
Maslow, B.-S. L., Guarnaccia, M. M., Ramirez, L., & Klein, J. U. (2020a). Likelihood of achieving a 50%, 60%, or 70% estimated live birth rate threshold with 1 or 2 cycles of planned oocyte cryopreservation. Journal of Assisted Reproduction and Genetics, 37(7), 1637–1643. https://doi.org/10.1007/s10815-020-01791-w
Share this
Recent Articles

Learn everything you need to know about IVF
Join the newsletter for IVF education, updates on new research, and early access to Alife products.



